 By Sarah Newman, MPH, Research and Evaluation Analyst, NACCHO
By Sarah Newman, MPH, Research and Evaluation Analyst, NACCHO
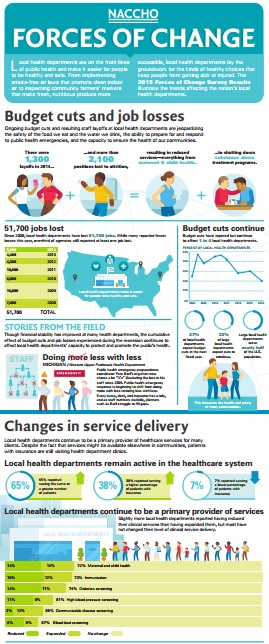
NACCHO has released the 2015 Forces of Change survey containing new findings on the forces that affect change in our nation’s local health departments (LHDs). Results show LHDs face challenges and opportunities as the public health and clinical care environments evolve.
Highlights
LHDs continue to experience budgetary challenges. Almost one-fourth of LHDs (23%) reported a lower budget in 2014 than the prior fiscal year and more (27%) expect budget cuts to continue into the next fiscal year. LHDs also continue to lose jobs; since 2008, LHDs have collectively lost 51,700 jobs due to layoffs and attrition. Likely as a result, LHD leaders value budget management skills in their professional public health staff: 80% rated budget management as very or extremely important for their staff.
These budget realities, as well as the implementation of the Patient Protection and Affordable Care Act (ACA) and changing community health needs, have had an impact on the type and scope of services LHDs provide. Some LHDs have decreased direct preventative clinical services to focus on population-based health activities, while others continue to provide these services in their communities. In order to continue to provide these essential clinical services, most LHDs (90%) have developed the capacity to bill third-party payers (public insurance providers such as Medicare and Medicaid and private insurers) for at least some services provided in LHD clinics.
In an increasingly competitive healthcare marketplace, findings show that LHDs are conveners that build, renew, and strengthen critical local relationships. More than half of LHDs (58%) are collaborating with non-profit hospitals on a community health needs assessment. In addition, LHDs are exploring ways to collaborate with primary care providers. More than half of agencies (61%) encourage primary care providers to use evidence-based public health services, such as interventions to reduce asthma triggers in children’s home environments. Fewer LHDs are engaged in new systems of care intended to improve patient outcomes and reduce costs: less than 10% are actively engaged in State Innovation Model activities, Patient-Centered Medical Homes, or Accountable Care Organizations.
Visit www.nacchoprofilestudy.org/forces-of-change to view an infographic of the findings and learn more.